
At CCCL stocks of chemotherapy drugs are so far still adequate, but uncertainty is growing. (Credit: João Sousa/L’Orient Today)
BEIRUT — As a physician treating Lebanon’s youngest cancer patients, Peter Noun always tries to remain positive. The tagline on the website of Kids First, the association he co-founded in 2005 to support children with cancer, is one of hope — “We Cancervive.”
Now, however, with Lebanon’s health care system crumbling, seeing the best in things is not so easy.
Stocks of medicines and equipment are running dry, highly skilled doctors and nurses are fleeing the country at record rates and health insurers are bowing under the pressure of a spiraling exchange rate.
“I really hate to be negative,” Noun, who works at the Saint George Hospital University Medical Center in Beirut (more commonly known as Mustashfa Roum), tells L’Orient Today, “but nowadays it is hard to be optimistic.”
Medicine: Relying on connections abroad
Over the last several months, pharmacy shelves and hospital storerooms have been emptied of medication as the central bank has allegedly delayed payments to foreign suppliers. The pharmaceutical importers syndicate has warned of “catastrophic” shortages by the end of July if the central bank fails to settle months' worth of unpaid invoices.
This means that parents, doctors and hospitals alike are scrambling to find the medication needed to treat children living with cancer, including chemotherapy.
“We have shortages of many drugs in Lebanon, and people are relying on connections with doctors or friends or relatives outside the country,” Noun says.
For families, he continues, this causes “a lot of anger, fear and disappointment.”
At Kids First, which covers the cost of care for families who cannot afford it, the team has also begun working to acquire drugs and medical supplies.
“Thank god, all our patients are taking their drugs, but only because the parents, myself, the NGO and the hospitals are working hard to get them,” Noun says. “We are exerting great efforts, just to get the essentials.”
At the Children’s Cancer Center Lebanon, which is linked to the American University of Beirut Medical Center and affiliated with St. Jude’s Children’s Research Hospital in Tennessee, stocks of chemotherapy drugs are so far still adequate, but uncertainty is growing.
“It’s definitely not as smooth as before and we have often had to wait for supplies,” says Dolly Noun, a pediatric hematologist-oncologist at AUBMC who treats patients at CCCL.
This is especially true of “regular medicines … such as antibiotics, pain medication or anti-nausea medication,” continues Dolly Noun, who hails from the same village as the Mustashfa Roum oncologist, but is not a close relative.
“When we prescribe something [to a patient], their family often has to search many pharmacies,” she says.
Just a few weeks ago, a patient at the CCCL fell unwell and was suffering from severe nausea and vomiting, Dolly Noun says. Staff prescribed four different medicines to treat him, but they were nowhere to be found, forcing him to come into the hospital and receive the drugs via an intravenous drip.
Yara, who is 12 years old, has been receiving treatment at the center for medulloblastoma, a form of brain tumor, for around a year.
“We come here once or twice a week, but sometimes the [chemotherapy] sessions take a while,” she says. During the COVID-19 lockdown, she used the long waits to participate in her school’s online classes.
When she grows up, she dreams of studying science, inspired by her older cousin, who is studying how to develop sustainable makeup products.
“She is working in a lab,” Yara says, smiling in CCCL’s colorful courtyard. “This is something I find really interesting.”
Her mother, Maya, says that while she considers her family to be relatively privileged, they have still faced issues with medicine shortages.
“We had some difficulty finding medicines, but luckily so far [CCCL] has always been able to give us another option,” she adds.
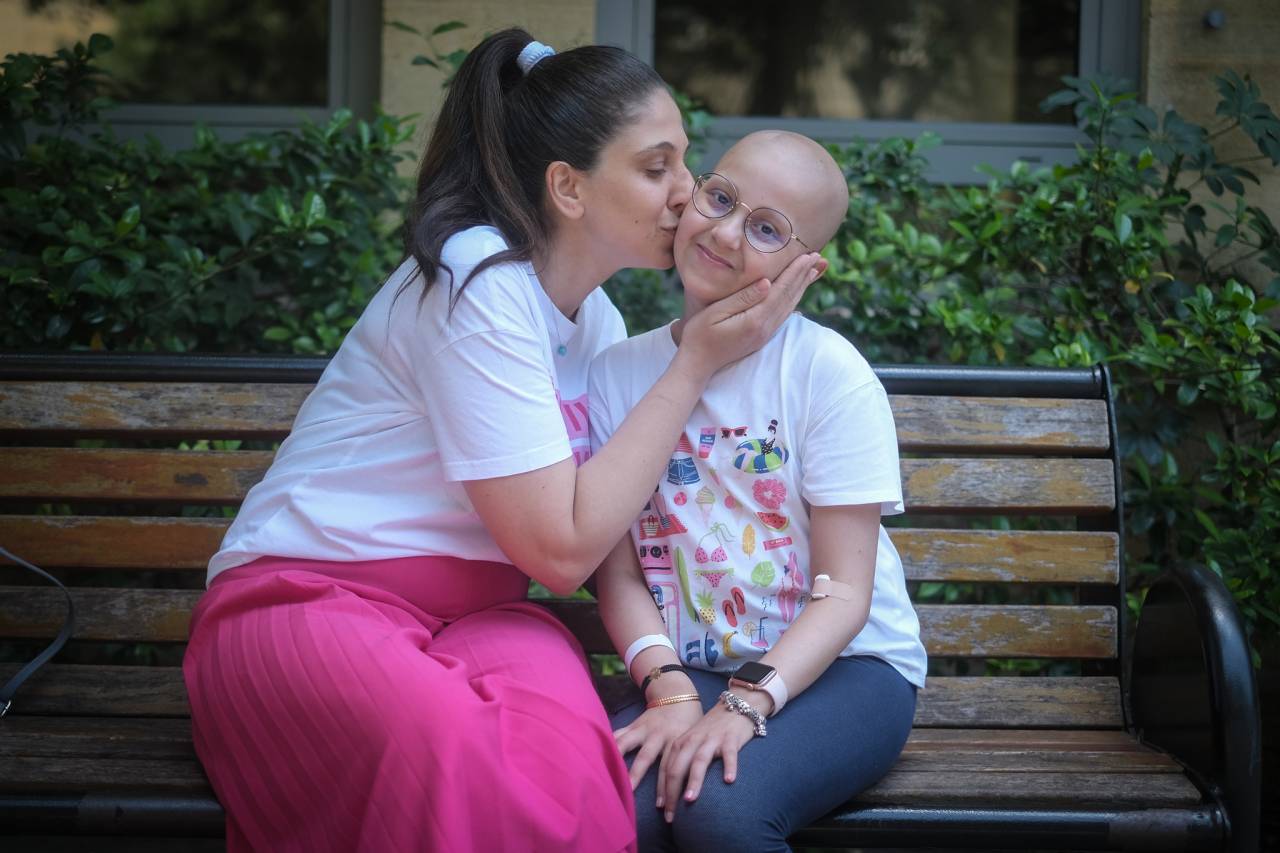 Yara and her mother sit in the garden at CCCL. (Credit: João Sousa/L’Orient Today)
Yara and her mother sit in the garden at CCCL. (Credit: João Sousa/L’Orient Today)
Sima Jeha, the Eastern Mediterranean Region director at St. Jude’s, with which CCCL has been partnered since 2002, warns that “collaboration with Lebanon has tragically shifted from transformative program building to responding to a country in crisis.”
“The concern is that a country where most children with cancer achieved cure is currently dealing with shortages — not only of medications, but of essential daily needs: water, food, electricity, fuel,” she adds.
Financial burden
The CCCL covers the cost of cancer care for some 540 children — 350 receive treatment from AUBMC and the rest at 13 other hospitals across the country. The CCCL’s yearly budget is around $15 million, with the average yearly cost of treatment per patient reaching $50,000.
Before the economic crisis, CCCL’s fundraising supervisor Lara Temsah Chaker explains, 80 percent of funds would come from donors and fundraising campaigns within Lebanon. But since then, the fundraising team has had to work harder to make up the money needed to keep the center running, especially after the COVID-19 pandemic limited the opportunities for traditional fundraising routes like gala dinners and events, and informal capital controls at Lebanese banks severely restricted cash withdrawals and transfers.
“The situation became unstable and people couldn’t take money out of the banks,” she says. “What little money they could get, they were unlikely to use that for donations.”
One of the issues facing the health care sector in Lebanon is growing gaps between what insurers, whether private or state bodies like the National Social Security Fund, will cover and the real-world cost of providing health care. While most insurers still provide coverage at the official rate of LL1,507.5, the cost of providing care has risen with the deterioration of the Lebanese lira, which is now trading just shy of LL20,000 on the parallel market. Therefore, some hospitals have begun charging for services at a rate of LL3,900 to the dollar or are asking patients to cover the gap left by insurers.
“At our center we cover the difference and we don’t ask the parents to pay anything,” Temsah Chaker says. “But this is another burden on us financially.”
Kids First is facing similar issues to CCCL, with previous fundraising activities becoming difficult due to COVID-19 restrictions and the deepening economic crisis.
“We do our best to cover the costs at the NGO, but it’s getting really complicated,” Peter Noun says, “Many people cannot afford to continue supporting themselves — how can they help others?”
Peter Noun’s ability to treat patients was also curtailed by the Aug. 4 Beirut port explosion, which destroyed Mustashfa Roum’s ninth floor pediatric oncology unit, which was on the side of the building facing the blast site.
“We are back to work but not in optimal conditions. We have to move from floor to floor as the construction happens,” he says. “Sometimes we have to use the same bed three times in a day to make sure all the patients get treated.”
“I cannot take many more patients because I don’t have the space,” Peter Noun continues, “but also because it costs much more and we have a lot of drugs and instruments lacking.”
 Before the economic crisis, CCCL’s fundraising supervisor Lara Temsah Chaker said, 80 percent of funds would come from donors and fundraising campaigns within Lebanon, but it has been much more difficult to raise money locally over the past two years. (Credit: João Sousa/L’Orient Today)
Before the economic crisis, CCCL’s fundraising supervisor Lara Temsah Chaker said, 80 percent of funds would come from donors and fundraising campaigns within Lebanon, but it has been much more difficult to raise money locally over the past two years. (Credit: João Sousa/L’Orient Today)
Fewer options
Shortages of medical essentials and the growing exodus of highly specialized health care workers mean that oncologists are concerned about the future of cancer care in Lebanon, which was for a long time famed as a regional hub for medical treatment.
“In a country where plain survival is so exhausting, the lengthy and complex treatment of cancer becomes simply unachievable,” Jeha says. “If the current situation is not immediately addressed the survival curves for children with cancer will show a gradual decline as was shown in other failing nations.”
A medical journal article published in January on the state of Lebanese cancer care said that due to Lebanon’s multiple crises, access to anticancer therapies has declined, particularly access to “novel and expensive drugs,” leading to a reliance on “classic, older and less effective medications for treatment.”
“The sad part is that not just the innovative, but even the traditional chemotherapy might be cut off,” Dolly Noun says. This may have an impact on the outcome of treatment, she warns.
In Lebanon, the average cure rate for childhood cancer is 80 percent, equivalent to rates in the US, the UK and Europe.
“We are still making this rate, but we are struggling,” Dolly Noun says. “Every time we lose a child, it’s really hard. I lose part of myself.”
Mustashfa Roum’s Peter Noun echoes her words. “With shortages of medicine, lack of funds, no vacancy of beds, we are decreasing the survival rate we had before,” he says. “It will take time [to be visible], but we can see it starting.”
“Generally the survival rate for pediatric oncology is very high. We must not lose this.”
Options even more limited in adult cancer care
Many of the challenges of pediatric cancer care also apply to adult cancer care, says Amal Nasser, a medical oncologist who runs clinics in Beirut and Tripoli.
“We are starting to face a crisis,” Nasser says. “We still have some reserves of chemotherapy and immunotherapy, but it’s difficult to get hold of them — we have to buy them from outside the country, with fresh dollars.”
While NGOs like CCCL and Kids First provide comprehensive coverage for children with cancer, options for adult cancer patients are more limited.
“Not all people are able to pay insurance any more,” Nasser says. “This means the burden [of increased health care costs] either falls on the Health Ministry, individual doctors or the patients themselves.”
The doctor says that where she can, she avoids placing extra charges on her patients, in some cases even personally footing the bill for the ever-widening gap between what is covered by insurance and the cost of treatment.
“On a personal and individual level we are finding solutions, but on a governmental level, there is nothing,” she says. “Cancer patients are facing death every moment, we cannot put these extra burdens on them.”
The Health Ministry, which provides health coverage for those who do not have private or public insurance, did not respond to requests for comment.
Nasser warns that state-of-the-art and innovative treatments are being affected by the crisis, and the range of available treatments is extremely limited.
One such treatment is precision medicine, where oncologists can pinpoint a particular chemotherapy to treat a specific cancer. “In the current crisis, we are not really able to do this,” she says.
The medical oncologist is also concerned over later diagnoses and detection of cancers due to delayed appointments during the COVID-19 pandemic and now because of shortages of laboratory reagents needed for tests.
Like for pediatric cancer patients, Nasser warns about the potential impact of the ongoing stresses on the health care system.
“So far, the survival rate has not been affected,” Nasser says. “But if the crisis does not have a solution, of course it will be.”





 Rubio condemns Iran's 'outrageous' attacks on Kuwait
Rubio condemns Iran's 'outrageous' attacks on Kuwait